Mammograms
October is Breast Cancer Awareness Month -- let's discuss the epidemiology of mammograms
October is Breast Cancer Awareness Month. It is an annual campaign to raise awareness about the impacts of breast cancer worldwide. According to the World Health Organization (WHO), 2.3 million women worldwide were diagnosed with and 685,000 women died from breast cancer in 2020.
Breast cancer is the most prevalent form of cancer among women globally.
The National Breast Cancer Foundation claims —
“This year we RISE to ensure every woman has access to the screening she needs and the support she deserves. When we RISE, we Rally In Screening Everyone.”
This claim/call to action begs several questions — first, what is screening?
Screening is a process of detecting breast changes or disease in a woman who has no signs or symptoms of disease. Quite simply — it is the detection of a tumor that cannot be felt.
Screening for breast cancer is usually done through mammography, which is an X-ray of the breast that can detect breast cancer in its early stages.
Who Should be Screened?
Here’s a question with no simple/clear answer. The U.S. Preventive Services Task Force recommends breast cancer screening every two years for women aged 50-74. The American Cancer Society recommends that breast cancer screening (with mammography) should begin at age 45 with an option to begin at age 40.
What’s someone in their mid-40s (like me) supposed to do?
And why are the recommendations different?
I believe that all individuals who want to screen for breast cancer (but especially those in their 40s) need to do two things — first, they must understand the underlying epidemiology that has led to the differing recommendations. And second, individuals need to talk with their primary care providers about the risks vs. benefits of a mammogram and their own individual risks for developing breast cancer.
Let’s start by talking about the epidemiology (I’m in my happy place now!) —
A mammogram, like every other screening test, is NOT perfect.
We know from years of breast cancer screening, diagnosis, and research that the sensitivity of a mammogram is 87% and the specificity of a mammogram is 89%.
The sensitivity of a screening test is the ability of the test to correctly identify individuals who truly have breast cancer. This means that a mammogram will correctly identify an individual who has breast cancer 87 times out of 100. In terms of accurately identifying small tumors, the mammogram performs at a B/B+ level.
The specificity of a screening test is the ability of the test to correctly identify individuals who truly do not have breast cancer. This means that 89% of the time a mammogram will correctly identify women who truly do not have breast cancer. Here the mammogram is performing at a solid B+ level.

Sensitivity & specificity are measures of how well a screening test performs. These measures are all about the mammogram’s performance. Sensitivity & specificity do NOT answer the key question that every individual having a mammogram wants to know which is —
what is the probability of having breast cancer given a positive screening test?
We can use the sensitivity and specificity of a mammogram (which quantifies the mammogram’s accuracy) and the prevalence of disease to calculate the —
POSITIVE PREDICTIVE VALUE
The positive predictive value or PPV of a mammogram quantifies the proportion of individuals who have breast cancer given that they have had a positive (also known as an irregular)1 mammogram. The PPV can be thought of as a benchmark for how likely it is that a positive screen during a mammogram truly indicates the presence of breast cancer.
Determining the PPV of a mammogram requires that we know three pieces of information: (1) sensitivity, (2) specificity, and (3) prevalence of disease.
Prevalence is the proportion of cases of disease in a specific population.
We know from public health surveillance data that the prevalence of breast cancer increases with age. There are more cases of breast cancer in the population of women who are 60 years of age and older compared to women who are less than 45 years. Given that prevalence increases with age, the value of a mammogram increases with age. In fact, women (biologic females) ages 50-74 benefit the most (as a collective group) from mammography.
Let’s look at an example — suppose you are like me and are in your mid-40s. And suppose you decide to get your first mammogram. And suppose following said mammogram you get a call from your beloved primary care provider telling you that your mammogram was positive (a bright, irregular spot was seen on your mammogram). You have screened positive for breast cancer. A flurry of activity happens — you get scheduled for a diagnostic ultrasound and you have to wait for a week all the while wondering do you have breast cancer.
The prevalence of breast cancer among females in their 40s is 9 percent. Given this, we know —

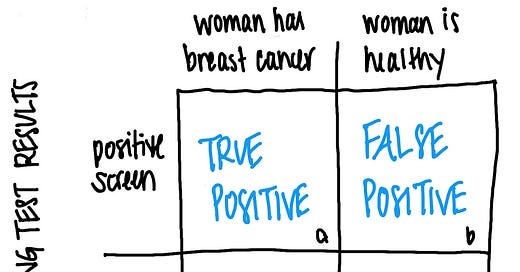
We calculate the PPV by taking the number of women who screen positive and truly have breast cancer (cell ‘a’) and dividing that by the total number of women who screen positive (the sum/total of cells ‘a’ + ‘b’). In this example it is 78.3/178.4 = 0.44.
The positive predictive value of my mammogram is 44%. This means that given that I’ve screened positive for breast cancer via a mammogram and I am in my mid-40s, the likelihood that I have breast cancer based on my mammogram results is 44%. More likely than not, I don’t have breast cancer. Despite the fact that I screened positive via mammogram. My screen was a false positive.
On the other hand, suppose you pull a 65-year-old female off the street, she has a mammogram, and she also receives the news that the screen was positive. Like me, the 40-something female, this 65-year-old is wondering do I have breast cancer.
The prevalence of breast cancer among females in their 60s is about 15%. Given this, we know —

We calculate the PPV by taking the number of women who screen positive and truly have breast cancer (cell ‘a’) and dividing that by the total number of women who screen positive (the sum/total of cells ‘a’ + ‘b’). In this example it is 130.5/224 = 0.58.
The positive predictive value of a mammogram of a 65-year-old woman is 58%. This means that given that she has screened positive for breast cancer via a mammogram the likelihood that she has breast cancer is 58%.
There is great harm in telling a woman she might have breast cancer when in fact she does not have breast cancer. There is emotional and mental stress, time needed for additional medical tests, and great cost to the individual (~$800 per person).
However, there is great harm — including increased mortality and more complicated/aggressive treatment protocols — for individuals who do not catch cancer in its early stages.
There are significant risks and benefits of using mammography as a screening test.
Do you risk telling someone they might have breast cancer when they do not? at the expense of missing a handful of true breast cancer cancers that are discovered via mammograms? or do you look at the PPV and say it is too low (a failing grade at 44%) to be used accurately and ethically to screen for breast cancer in all women in their 40s?
The American Cancer Society believes the benefit of screening all women in their 40s and diagnosing cases (despite the fact there are very few cases among individuals in their 40s) far outweighs the fact that many women will have a false positive mammogram. The U.S. Preventive Services Task Force does not believe that screening all women in their 40s is worth that risk. The Task Force is looking at the positive predictive value of a mammogram, which is less than 50%, and saying we get it wrong more than 50% of the time; this is not sound preventive medicine.
No one is right. Neither is wrong. As a screening test the mammogram is (kind of) lousy, but it is the best we have.
Mammography does help identify cancer before a tumor can be felt. But it is far from perfect. There are risks and benefits to being screened in your 40s. Once an individual turns 50 and the prevalence of breast cancer increases in their age group, the value of a mammogram increases.
But still, the positive predictive value is only 58%.
This means 42% of individuals who have a positive screen will NOT have breast cancer. Whether you can emotionally handle, afford, or access the diagnostic tests needed to know if the screen is a true positive or false positive, is a conversation that needs to happen with a primary care provider.
Personally — I took the middle road. After consulting with my physician, I decided to have my first mammogram in my mid-40s. Like many women my age, my first mammogram came back positive. The X-ray showed a white area on the right side close to my armpit. I received a scary call from my physician. I had to wait a week for an ultrasound and then another day or two for the results. Only to find out that I was one of many false-positive mammograms.
Was it stressful? Yes.
Am I grateful to have the peace of mind that it was not breast cancer? Absolutely.
Was I comfortable forgoing a mammogram until my 50th birthday? Obviously, not. However, in my mind, the statistics discussed above were on repeat. The likelihood of me having breast cancer in my 40s is low. The likelihood that my mammogram was a true positive was also low. But I needed to know.
So I decided to get a mammogram in my 40s. And now that I’ve had one positive mammogram, I have to get checked annually (next month - stay tuned…).
Did I make the ‘right’ decision? I don’t know.
What do I know? We need to advocate for better screening tests. We need a mammogram (or another screening tool) that has a sensitivity and specificity greater than 90%. We cannot settle for screening tools that only work part of the time/when prevalence is high if we want to be able to detect, diagnose, and treat breast cancer. And improve the outcomes of individuals with breast cancer.
Please note — if you are at high risk for developing breast cancer (you have the BRCA gene or have a family history of breast cancer), screening is recommended that you receive an annual mammogram in your 30s.
Questions?
Side note — a positive breast cancer screen = bad/something was seen on the X-ray that could be cancer. A negative breast cancer screen = good/the X-rays was clear. This phrasing is confusing and really should be changed. Comprehending a positive screen as bad and a negative as good is counterintuitive. We can do better, especially in the midst of screening test that causes anxiety.





Thank you so much for this! There are no clear answers for every person, but this is very helpful information to think through doing the mammogram or not. I'm curious why the screening procedure does not to use the more powerful ultrasound rather than the xray. It seems like that's a route to improved accuracy in detection if it's the next step after a positive xray. I'm sure it comes down to financial costs...